Plantar Fasciitis Treatment
Anyone who spends all day on their feet will tell you that they go home exhausted at the end of the day. Teachers, nurses, hair-dressers, athletes, factory workers, anyone who spends a majority of their time standing knows just how painful the end, and often the start, of the day can be.
If you are interested in helping others through massage therapy be sure to fill out the form on this page to get more information about our wellness programs.
Scroll to the bottom of this post to watch the full video on plantar fasciitis treatment.
What is Plantar Fasciitis?

Individuals whose careers and hobbies require constant standing may suffer from Plantar Fasciitis. This condition is one of the most common causes of heel pain and usually results from inflammation and stress of the plantar fascia, the ligament that connects your heel to your toes and supports the arch of your foot. Wellness instructors from the massage therapy schools at Fremont University have seen this type of sports injury far too many times. If you are experiencing heel pain, it could be you are experiencing a case of Plantar Fasciitis.
While Plantar Fasciitis is more common in individuals ages 40 to 60, it can also occur in younger people who spend a good portion of their time on their feet. The discomfort in your heel(s) may be noticed mostly while walking after periods of rest, standing on hard surfaces or climbing stairs. If you think you might be experiencing Plantar Fasciitis, here are a few things to be aware of.
Symptoms:
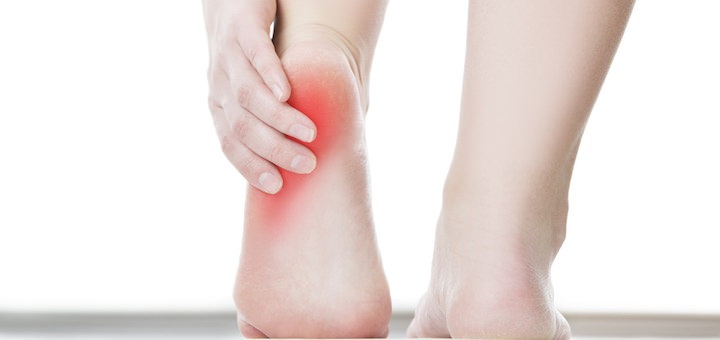
Some symptoms to keep in mind if you think you are experiencing Plantar Fasciitis are as follows: pain in your heel(s) after getting out of bed or sitting for a long period of time – this pain may decrease as the day goes on- pain after standing for extended periods of time and even discomfort after exercise. It is important to remember that discomfort will not usually occur during any kind of activity, but afterward and following periods of rest. If you notice discomfort in your heel after sitting for an extended period of time or when getting out of bed in the morning, you should start thinking about when the pain began and what might be causing the discomfort.
Causes:

Plantar Fasciitis commonly results from straining and tears in the plantar fascia ligament. Such stress can be caused by a number of things, such as excessive pronation (feet rolling inward) while you walk, extremely high or flat arches and past injuries. If you are an athlete, injuries or sports such as long distance running, jumping and high impact dance, especially on hard surfaces, might be the cause of your discomfort. Remember that it is not only athletes that can develop Plantar Fasciitis, even something as simple as wearing shoes that do not fit you properly, walking in a unique way or being overweight can cause heel pain.
[contact-form-7 id=”31766″ title=”Be a better person of your self form” html_class=”gray-form”]
If you have already developed Plantar Fasciitis it is important to be aware that attempting to adjust your walk to compensate for an injury, ill-fitting shoes or pronation can do more harm than good. If you are trying to adjust for some of these causes, you might start experiencing back pain, hip problems or discomfort in your knees. If you noticed that you are experiencing heel pain and think you have an idea of what may have led to your discomfort, it is a good idea to consult a doctor.
Diagnosis:
When you visit a doctor to discuss the possibility of Plantar Fasciitis, he or she will ask you a number of questions about past pain, injuries, health and any kind of physical activities you may take part in. Often doctors will make a diagnosis based on your answers and a brief examination of your foot. Doctors will check different areas of your foot to determine where the most discomfort and tenderness might be and make a diagnosis based on your answers and the location of the pain. Invasive tests are rarely ever required, nor are imaging tests; your doctor might recommend an X-ray or MRI to ensure the pain is not caused by anything else, but more often than not such tests are not required.
Non-Invasive Treatments and Exercises:
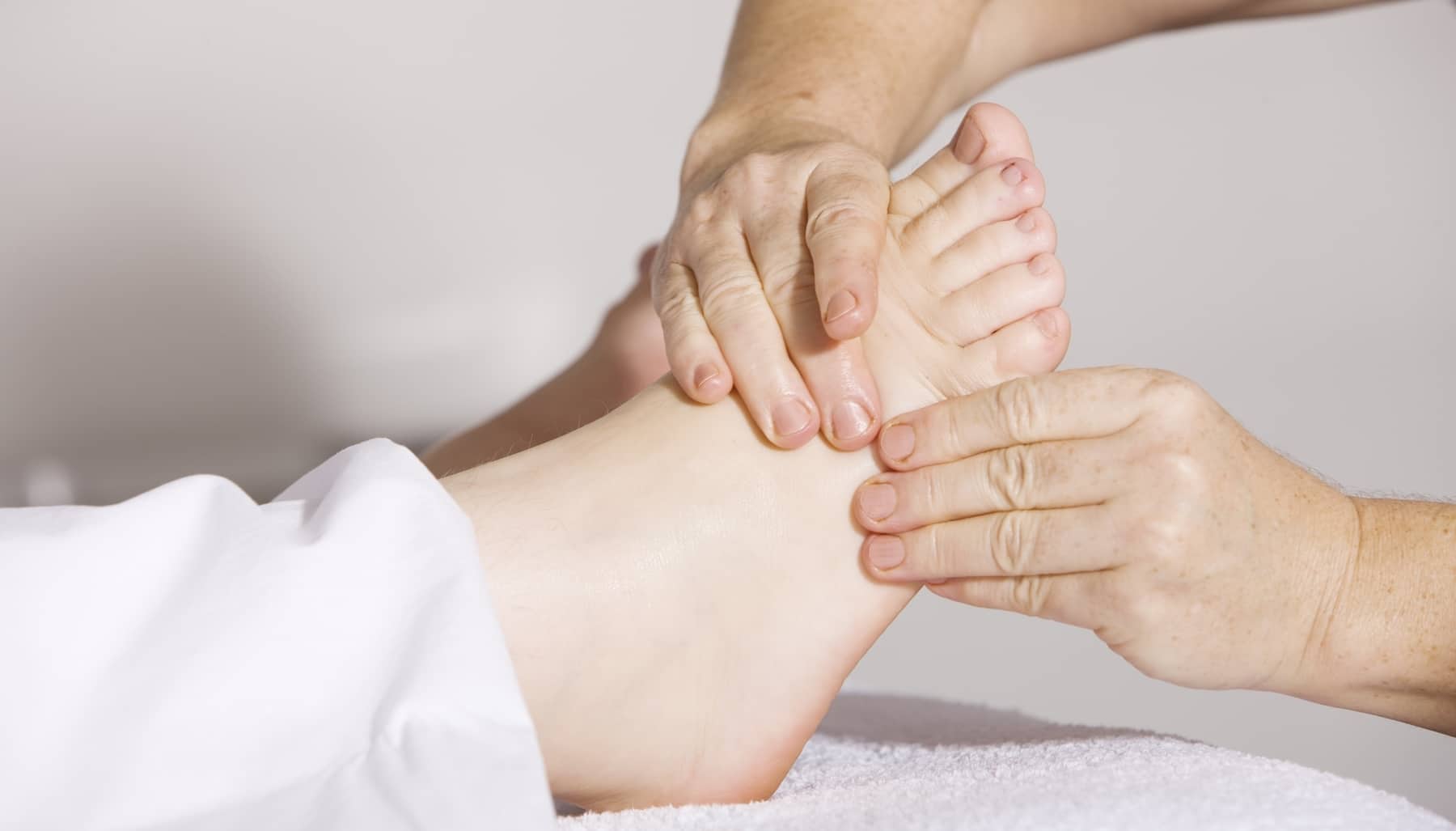
The best treatments for Plantar Fasciitis are non-invasive and very easy to perform at home. For example, maintaining a healthy weight can help ensure that Plantar Fasciitis does not worsen or continue. Some of the below are possible non-invasive treatments and exercises that might be used.
- If you and your doctor have agreed that weight is not a factor in your discomfort, rest is essential to ensuring that the muscle has time to heal. Rest your feet and reduce any activities that may be causing your discomfort, such as high impact exercise, standing for long periods of time or standing and walking on hard surfaces.
- Icing the irritated area can also ease pain and help recovery move along by reducing inflammation; alternating between heat and ice may also be helpful.
- Making sure the shoes you are wearing have proper support and cushioning will also ease the pain. If you find that your shoes are worn out or do not provide the support you need, invest in a new pair or two; a good shoe can work wonders.
- Applying athletic taping will also provide support to your foot. If none of these home remedies are working, your doctor might recommend night splints that stretch your arch while you sleep, or over the counter pain relievers such as Advil, Motrin or Aleve.
- Stretching can also help reduce pain and assist in recovery. Toe stretches in order to stretch the arch of your foot can help relieve pain, as can Calf Stretches or performing towel stretches throughout the day.
Massage Therapy Demonstration for Plantar Fasciitis
Invasive Treatments:
An article on Mayo Clinic.org discusses some more invasive treatments for Plantar Fasciitis. Invasive treatments are rare and are only recommended in cases where pain has not subsided after a year of rehabilitation. Injections of steroids have been prescribed, though such injections can weaken the plantar fascia further; extracorporeal shock wave therapy can be recommended but has not been shown to consistently improve a patient’s discomfort, while the Tenex procedure removes scar tissue of plantar fasciitis without surgery. Surgery is rarely performed for individuals with Plantar Fasciitis since it can weaken the arch in your foot; it is usually only resorted to if all other treatments have failed.
It is important to remember that recovery from Plantar Fasciitis can take several months to a year before any real improvement is noticeable. If you follow your doctor’s instructions and recommended exercises, you will slowly make improvements that will reduce pain and allow you to resume your normal lifestyle.
Want To Help Others Through Massage Therapy?
If you’re looking to help people through massage therapy be sure to fill out the form on this page to get more information. If you’re interested in scheduling a campus tour call Fremont University at (800) 373-6668 and ask to speak with an admissions representative.
*In no way does Fremont University promise or guarantee employment or level of income/wages. In no way is it recommended that you try to treat injuries by yourself. That should be done by a qualified professional. Before practicing any new modalities or techniques, check with your state’s regulatory authority to ensure they are within the state’s defined scope and standards of practice for therapy.

